Rejection Sensitivity vs Fear of Abandonment: A DBT-Informed Perspective on ADHD and BPD
Differentiating rejection sensitivity and fear of abandonment in ADHD and BPD, with evidence-based strategies from Dialectical Behaviour Therapy.
- Emotional pain triggered by perceived disapproval or rejection
- Disproportionate anger or shame in response to feedback
- Avoidance of failure or evaluation
- People-pleasing and perfectionistic tendencies
- Internal beliefs of being defective or unworthy
- Hypervigilance to signs of distance or detachment
- Idealisation followed by devaluation in relationships
- Reassurance-seeking and “testing” behaviours
- Intense anger, self-harm, or threats in response to perceived rejection
- Deep feelings of emptiness, insecurity, and identity confusion
| Feature | Rejection Sensitivity (ADHD) | Fear of Abandonment (BPD) |
|---|---|---|
| Core Concern | Perceived criticism or disapproval | Perceived or actual relational loss |
| Triggering Context | Evaluation, feedback, exclusion | Distance, change, or inconsistency in closeness |
| Primary Emotions | Shame, humiliation, rage | Panic, fear, despair |
| Behavioural Responses | People-pleasing, avoidance, withdrawal, outbursts | Clinginess, testing, self-harm, controlling behaviour |
| Underlying Schema | “I am inadequate/unlikeable” | “People I love will leave me” |
| Neurocognitive Basis | Emotional impulsivity, rejection hypersensitivity in ADHD circuitry | Hyperactivation of attachment and threat systems in BPD |
Some individuals present with both ADHD and BPD traits, in which case rejection sensitivity and abandonment fear may interact. In such presentations, the emotional volatility may be compounded, requiring comprehensive and carefully tailored intervention.
Treating Rejec tion Sensitivity and Fear of Abandonment with DBT
Dialectical Behaviour Therapy was originally developed for individuals with BPD who experience chronic emotion dysregulation and suicidal behaviour. However, DBT has also been successfully adapted for adults with ADHD, particularly those with difficulties managing emotional intensity and interpersonal stress.
DBT addresses the cognitive, behavioural, and emotional elements that contribute to rejection sensitivity and abandonment fear. It combines acceptance strategies with behaviour change techniques, creating a structured and validating therapeutic environment.
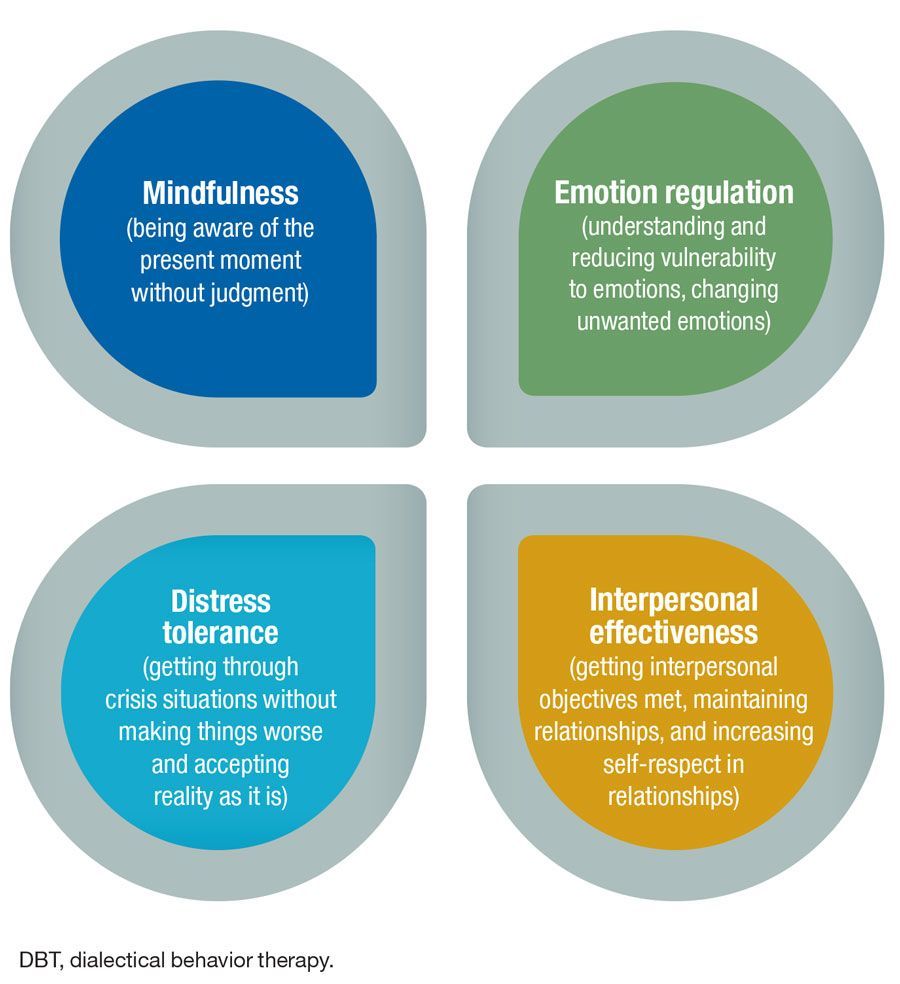
1. Mindfulness
Mindfulness teaches individuals how to observe and describe their internal experiences without judgement. This helps people identify emotional triggers and create space between stimulus and response.
Applications include:
- Recognising early signs of emotional activation
- Observing thoughts without automatically believing them
- Developing present-moment awareness during interpersonal stress
- Mindfulness has been shown to reduce emotional reactivity and improve executive functioning in individuals with both ADHD and BPD.
2. Emotion Regulation
Emotion regulation skills help individuals identify, understand, and manage their emotions more effectively. This includes strategies such as:
- Labelling emotions accurately
- Reducing vulnerability (e.g., through sleep, nutrition, exercise)
- Checking the facts behind emotional reactions
- Applying opposite action when appropriate
These skills are especially important for reducing the shame, anxiety, and anger that characterise both RSD and abandonment distress.
3. Distress Tolerance
When emotions become overwhelming, distress tolerance skills enable individuals to survive the moment without engaging in impulsive or harmful behaviours.
Common strategies include:
- Self-soothing with sensory-based grounding
- Crisis survival skills such as TIP (temperature, intense exercise, paced breathing)
- Radical acceptance of painful realities that cannot be changed in the moment
- These skills reduce the likelihood of escalation during episodes of rejection or relational stress.
4. Interpersonal Effectiveness
Individuals with rejection sensitivity or abandonment fear often struggle to communicate assertively or maintain relational boundaries. DBT offers a structured framework for:
- Asking for needs clearly (DEAR MAN)
- Maintaining self-respect (FAST)
- Strengthening relationships through validation and empathy (GIVE)
These skills support relational stability and reduce the cycle of overreacting, withdrawing, or pushing others away.
Evidence for DBT in ADHD and BPD
DBT has an extensive evidence base for the treatment of BPD. Research shows reductions in self-harm, emotional dysregulation, and relationship instability following DBT participation.
In recent years, DBT-informed interventions have been adapted for adults with ADHD. Emerging evidence suggests that DBT skills training improves emotion regulation, executive function, and interpersonal outcomes in ADHD populations.
While further research is needed, current findings support DBT as an effective transdiagnostic treatment for emotion regulation difficulties.
Final Thoughts
Rejection sensitivity and fear of abandonment are often misunderstood, even among mental health professionals. They are not signs of weakness or immaturity. Rather, they reflect deep emotional vulnerability shaped by neurobiology, history, and relational context.
With the right support, individuals can learn to understand their emotional responses, manage triggers, and build relationships based on trust and stability. DBT offers a practical and compassionate framework for this work. It equips people with the skills needed not only to survive emotional pain, but to move forward with greater clarity, resilience, and self-worth.
If you are struggling with overwhelming emotional reactions, or if you relate to what has been described here, we encourage you to reach out. Support is available, and healing is possible.
To learn more about our DBT programs and Individual Therapy feel free to contact us at reception@wise-mind.com.au or by phone on 2114 7153.
Wise-Mind Matters