Autistic Burnout: Why Rest Is Not Avoidance
Autistic burnout is often misunderstood. From the outside, it may look like withdrawal, avoidance, low motivation, irritability, depression, disorganisation, or a sudden reduction in functioning. A person who previously managed work, study, parenting, relationships, appointments, social events, or daily tasks may begin to struggle with things they used to do. They may need far more rest, avoid social contact, lose tolerance for noise or demands, become more emotionally reactive, or find that ordinary routines suddenly feel unmanageable.
Because autistic burnout can affect functioning so significantly, it is often mistaken for laziness, avoidance, non-compliance, lack of resilience, or “not trying”. This is both inaccurate and harmful. Autistic burnout is not a character flaw. It is often the result of prolonged stress, sensory overload, masking, unmet needs, excessive demands, insufficient recovery time, and the ongoing effort of navigating environments that do not adequately fit the person’s nervous system.
For many autistic people, rest is not indulgence. It is not giving up. It is not avoidance. Rest is often a necessary part of nervous system recovery.
At Wise-Mind DBT Brisbane, we recognise that emotional regulation support for autistic people must be neurodiversity-affirming. This means we do not treat autistic distress as something to be hidden, suppressed, or “pushed through” for the comfort of others. Instead, we aim to understand what the distress is communicating, what demands have exceeded capacity, and what skills, boundaries, and environmental changes may support a more sustainable life.
What Is Autistic Burnout?
Autistic burnout is a state of significant physical, emotional, sensory, and cognitive exhaustion. It is commonly associated with long-term stress and the cumulative cost of functioning in environments that require constant adaptation. While every autistic person’s experience is different, burnout often involves a marked reduction in capacity.
A person may find it harder to speak, make decisions, process information, manage transitions, tolerate sensory input, maintain routines, attend appointments, respond to messages, work, study, or participate in relationships. They may feel as though skills they previously relied on are no longer available. This can be frightening, especially for people who have built their identity around being capable, reliable, high-achieving, or self-sufficient.
Autistic burnout can be especially confusing when the person has been masking for many years. From the outside, they may have appeared to be coping. Internally, however, they may have been using enormous effort to manage sensory overload, social expectations, executive functioning demands, emotional labour, and the pressure to appear “fine”. Burnout can occur when that effort is no longer sustainable.
It is important to understand that autistic burnout is not simply being tired after a busy week. It is often deeper and more prolonged. It may require significant reduction in demands, changes to routines, increased support, and careful recovery over time.
Why Autistic Burnout Happens
Autistic burnout often develops when the demands placed on a person repeatedly exceed their available capacity. This may occur because of external demands, internal pressure, or both.
External demands might include work expectations, study requirements, parenting responsibilities, social obligations, financial stress, appointments, relationship conflict, sensory environments, unclear communication, or frequent changes in routine. For autistic people, these demands may require additional effort because they often involve sensory processing, executive functioning, social interpretation, transitions, and emotional regulation.
Internal pressure can also contribute. Many autistic people have spent years being told, directly or indirectly, that their needs are inconvenient or excessive. They may learn to push through discomfort, hide distress, ignore sensory pain, suppress stimming, force eye contact, over-prepare for conversations, and say yes when they need to say no. Over time, this can create a pattern of chronic self-overriding.
Masking is a major contributor to burnout. When someone is constantly monitoring how they appear, adjusting their communication, hiding distress, and performing acceptability, the nervous system may never receive adequate recovery time. The person may keep functioning outwardly until they reach a point where functioning drops suddenly.
Burnout may also occur after major life transitions. Starting university, changing jobs, becoming a parent, ending a relationship, moving house, receiving a diagnosis, managing grief, or navigating increased responsibilities can all increase demand. Even positive changes can be exhausting if they require significant adjustment.
Burnout Is Not Avoidance
Avoidance is usually a behaviour that reduces distress in the short term by moving away from something difficult, feared, overwhelming, or uncomfortable. Avoidance can become problematic when it narrows life, prevents important action, or increases distress over time.
Autistic burnout is different. Burnout is not simply a refusal to engage. It is often a reduction in capacity caused by prolonged overload. A person in burnout may not be avoiding because they do not care. They may be unable to engage in the usual way because their nervous system, cognitive resources, sensory tolerance, and emotional capacity are depleted.
This distinction matters clinically and relationally. If burnout is treated as avoidance, the person may be pressured to push harder, increase exposure, attend more, socialise more, or “get back to normal” before they have recovered. This can worsen burnout and deepen shame.
A more accurate question is not, “Why are you avoiding?” but “What has exceeded capacity, and what would support recovery?”
This does not mean all withdrawal is automatically helpful. Sometimes people do avoid tasks or conversations in ways that create further difficulties. However, in autistic burnout, rest and reduced demand are often necessary before problem-solving can be effective. The task is to distinguish between skilful recovery and fear-driven avoidance, rather than assuming all rest is avoidance.
The Cost of Pushing Through
Many autistic people have become skilled at pushing through. They may have learned to attend the event, complete the shift, meet the deadline, answer the messages, tolerate the noise, manage the conversation, and appear calm even when internally overwhelmed. This can be necessary in some environments, especially when there are financial, relational, or safety pressures.
However, pushing through has a cost. The body keeps score of effort, even when others do not see it. A person may be able to get through a demanding day, but then lose the ability to cook dinner, shower, speak, sleep, or regulate emotions afterwards. They may attend a social event, then need days to recover. They may manage work by masking all day, then experience meltdowns or shutdowns at home.
When pushing through becomes the default, the person may lose touch with early warning signs. They may not notice overload until they are already in crisis. They may interpret rest as failure because they have been rewarded for endurance. They may feel guilty for needing recovery time, even when their body is clearly signalling depletion.
DBT can help here, but only when adapted appropriately. The goal is not to become better at pushing through burnout. The goal is to develop mindfulness of capacity, use Wise Mind to respond earlier, and make changes that reduce the need for constant survival mode.
Signs of Autistic Burnout
Autistic burnout can look different for each person, but common signs include exhaustion, increased sensory sensitivity, reduced ability to manage daily tasks, more frequent meltdowns or shutdowns, difficulty speaking or communicating, increased need for solitude, executive functioning difficulties, emotional dysregulation, loss of motivation, sleep disruption, and reduced tolerance for change.
Some people notice that previously manageable tasks become much harder. Grocery shopping, making phone calls, replying to emails, attending appointments, cooking, cleaning, decision-making, or transitioning between activities may suddenly require enormous effort. Others notice that social interaction feels unbearable, even with people they care about.
Burnout may also affect identity and self-esteem. A person may feel confused or ashamed because they “used to be able to do more”. They may compare themselves to past versions of themselves or to other people who appear to cope more easily. This shame can intensify burnout because it adds emotional suffering to an already depleted system.
Recognising burnout early is important. The earlier a person notices that capacity is dropping, the more likely they are to prevent a deeper collapse.
Rest as a Regulation Strategy
Rest is often spoken about as if it is passive, but in burnout recovery, rest can be an active regulation strategy. Rest allows the nervous system to reduce activation, process accumulated stress, recover from sensory load, and rebuild capacity.
For autistic people, rest may not look like simply doing nothing. It may involve low-demand time, predictable routines, reduced social interaction, special interests, sensory-friendly environments, comfortable clothing, quiet spaces, movement, deep pressure, sleep, reduced decision-making, or time away from performance. Rest should be understood in terms of what actually restores the person, not what other people think should be relaxing.
Some people rest best through solitude. Others need co-regulation with a safe person who does not require much from them. Some need silence. Others need familiar background sound. Some need darkness or low light. Others need movement, pressure, or repetitive activity. A neurodiversity-affirming approach does not prescribe rest in one form. It helps the person identify what genuinely supports recovery.
Rest also needs to be protected from guilt. If a person spends their entire rest period criticising themselves for resting, the nervous system may not recover. Self-validation is therefore essential. The person may need to remind themselves that rest is not laziness. It is part of responding effectively to burnout.
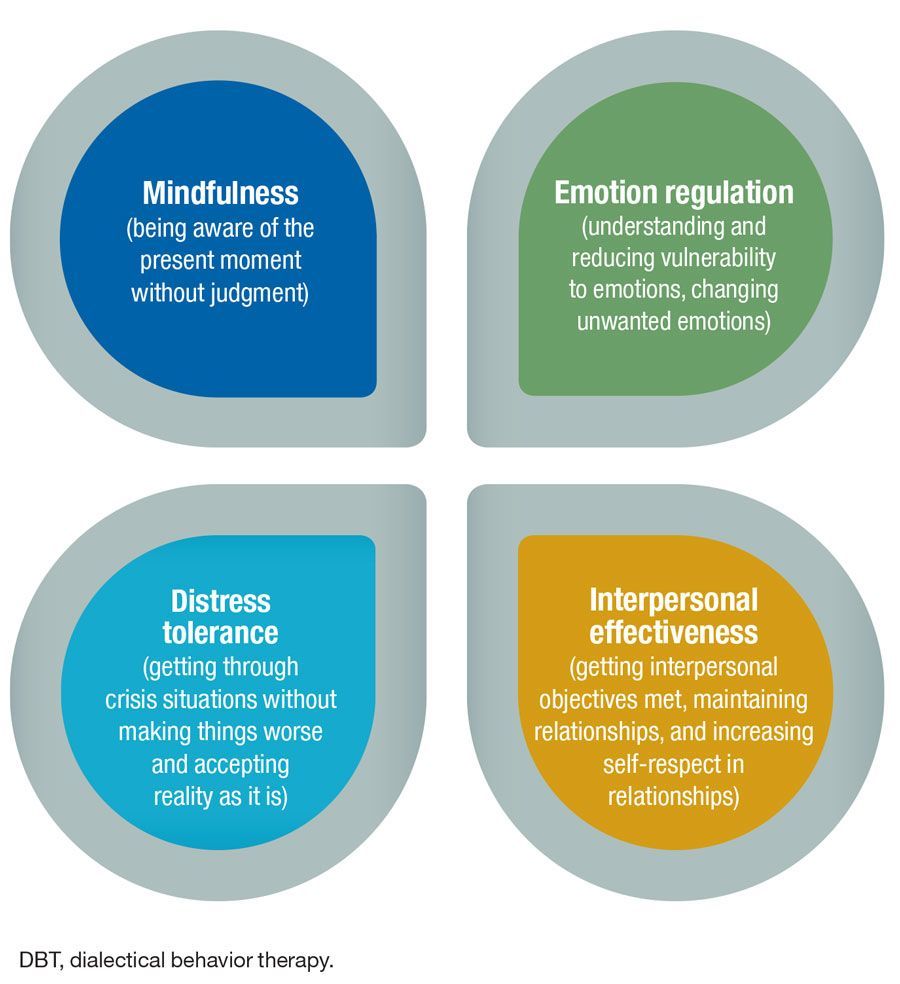
DBT, Burnout, and Wise Mind
Wise Mind is a central DBT skill that involves integrating emotional information and reasonable information. In autistic burnout, Wise Mind may help a person make decisions that respect both current limitations and longer-term values.
Emotion Mind might say, “I cannot do anything. I should cancel everything forever.” Reasonable Mind might say, “I have responsibilities, so I should ignore how I feel and push through.” Wise Mind looks for a more balanced truth. It might recognise that the person is genuinely depleted and needs reduced demands, while also identifying the next small responsibility that cannot be ignored.
Wise Mind might support decisions such as contacting work to discuss adjustments, rescheduling non-urgent appointments, asking for help with meals, reducing social commitments, creating a sensory recovery plan, or breaking necessary tasks into smaller steps. It might also recognise when rest is the most effective action.
This is important because burnout recovery often requires both acceptance and change. Acceptance means recognising that capacity is currently reduced and that forcing the old level of functioning may cause further harm. Change means making practical adjustments, seeking support, and slowly rebuilding sustainable routines.
Mindfulness of Capacity
Mindfulness in DBT is often described as paying attention to the present moment. For autistic burnout, mindfulness can include paying attention to capacity. This means noticing early signs of overload before the system collapses.
Many autistic people have learned to ignore internal cues. They may not notice hunger, fatigue, sensory pain, emotional escalation, or social exhaustion until the signals become severe. Mindfulness of capacity involves slowly rebuilding awareness of these cues.
This might include noticing when sound becomes sharper, when speech becomes harder, when decision-making slows, when irritability increases, when lights feel more painful, when the body feels heavy, or when the thought of one more demand feels unbearable. These are not signs of failure. They are information.
The aim is to respond earlier. If the person notices overload at a four out of ten, they may be able to take a sensory break, reduce demands, eat, rest, move, or ask for support. If they only notice at a nine out of ten, shutdown or meltdown may already be close.
Mindfulness of capacity helps shift the question from “How much can I force myself to tolerate?” to “What is my nervous system telling me, and what would be effective now?”
Distress Tolerance Without Forcing Endurance
Distress tolerance is a DBT skill set designed to help people get through painful moments without making things worse. In autistic burnout, distress tolerance can be useful, but it must be applied carefully.
Distress tolerance should not be used to force an autistic person to remain in overwhelming, inaccessible, or harmful environments. If a room is too loud, if a social demand is beyond capacity, if speech is no longer accessible, or if sensory overload is escalating, the skilful response may be to leave, reduce input, use headphones, communicate a need, or stop the activity.
In this context, “not making things worse” may mean preventing deeper overload. It may mean taking a break before shutdown. It may mean using written communication instead of speech. It may mean declining a commitment that would push the person further into burnout. It may mean choosing rest rather than forcing productivity.
Distress tolerance may also help when the person feels guilt or anxiety about resting. The distress may not come from the rest itself, but from internalised beliefs about being lazy, difficult, or disappointing others. Skills such as grounding, self-soothing, paced breathing, and self-validation can help the person tolerate those feelings without abandoning their recovery needs.
Emotion Regulation and Reducing Vulnerability
DBT emotion regulation includes reducing vulnerability to emotional overwhelm. For autistic people in burnout, this often requires attending to the conditions that make overload more likely.
Sleep, food, hydration, medication, movement, illness, pain, and substance use all matter. However, autistic vulnerability reduction also needs to include sensory load, social load, transition demands, masking demands, executive functioning demands, and recovery time.
A person may need to reduce the number of appointments in a week, simplify meals, use grocery delivery, ask for written instructions, create predictable routines, reduce exposure to overwhelming environments, wear sensory-friendly clothing, use noise-cancelling headphones, or build recovery time after work or social contact. These are not indulgences. They are regulation supports.
Emotion regulation also involves building positive and meaningful experiences, but during burnout this needs to be paced. A person may not have capacity for large goals or demanding activities. Small, restorative, low-pressure experiences may be more appropriate. This could include engaging with a special interest, spending time with a safe person, being in nature, listening to familiar music, or completing one achievable task.
The aim is not to force improvement quickly. The aim is to reduce vulnerability and rebuild capacity gradually.
Interpersonal Effectiveness and Communicating Burnout
Communicating burnout can be difficult, particularly when other people have only seen the person’s masked functioning. Family members, partners, employers, teachers, or friends may not understand why the person suddenly needs more rest or fewer demands. They may interpret withdrawal as rejection, disinterest, irresponsibility, or avoidance.
DBT interpersonal effectiveness skills can help the person communicate needs clearly while maintaining self-respect. This might involve explaining that capacity is reduced, asking for specific adjustments, setting limits around social demands, or requesting written communication. It may also involve saying no without over-explaining or apologising excessively.
For example, instead of trying to justify every detail of burnout, a person may learn to state that they are currently experiencing reduced capacity and need to limit commitments for a period of time. They might ask for practical support, such as help with meals, reduced noise, more notice before changes, or flexibility around attendance.
Communication does not guarantee that others will understand. However, clear and boundaried communication can reduce confusion and help protect the person from further overextension.
Rest, Responsibility, and the Dialectic
One of the challenges in burnout recovery is holding the dialectic between rest and responsibility. Some people fear that if they allow themselves to rest, everything will fall apart. Others may be so depleted that even small responsibilities feel impossible. Both experiences can be real.
DBT helps by holding two truths at the same time. A person may genuinely need rest, and there may still be responsibilities that require attention. A person may not be able to function at their previous level, and they may still be able to take one small step. A person may need support, and they may still have agency.
This dialectic prevents burnout recovery from becoming all-or-nothing. The goal is not to abandon life completely or push through as though nothing has changed. The goal is to identify what is essential, what can be reduced, what can be delegated, what can be delayed, and what supports are needed.
Sometimes Wise Mind says, “Rest now.” Sometimes it says, “Do the smallest necessary step, then rest.” Sometimes it says, “Ask for help.” Sometimes it says, “This expectation is not sustainable and needs to change.”
Rebuilding After Burnout
Recovery from autistic burnout is often gradual. It may require more time than the person expects or wants. This can be frustrating, especially for people who are used to functioning at a high level or meeting others’ expectations.
Rebuilding should be paced. Returning too quickly to the same demands that caused burnout can lead to relapse. Instead, the person may need to slowly reintroduce activities while monitoring capacity carefully. This may involve shorter work hours, reduced social commitments, more predictable routines, sensory accommodations, support with executive functioning, and ongoing recovery time.
It is also important to learn from the burnout. What contributed to it? Was there too much masking? Too little rest? Too many transitions? Too much sensory input? Too many social demands? Too much ambiguity? Too much emotional labour? Too little support? Burnout is not only something to recover from. It is also information about what needs to change.
Rebuilding is not about returning to the exact same life if that life was unsustainable. It may involve building a life that better fits the person’s autistic needs.
Supporting Someone in Autistic Burnout
If someone you care about is experiencing autistic burnout, it is important to believe them when they say they are depleted. They may not be able to explain everything clearly, especially if communication is affected. They may need fewer questions, more practical support, reduced sensory input, and patience.
Helpful support may include offering concrete assistance rather than vague encouragement. This might mean helping with meals, transport, administration, childcare, cleaning, scheduling, or reducing demands. It may mean accepting written communication, giving notice before changes, avoiding pressure to socialise, and not interpreting shutdown as rejection.
It is also important not to respond with shame. Statements that imply laziness, avoidance, selfishness, or overreaction can deepen burnout and make the person less likely to ask for help. A more helpful stance is curiosity: “What is too much right now?” “What would reduce demand?” “What support would make today easier?”
Support does not mean removing all responsibility forever. It means helping the person recover enough capacity to participate in life in a sustainable way.
Rest Is Part of Building a Life Worth Living
DBT often speaks about building a life worth living. For autistic people, a life worth living cannot be built on constant masking, chronic overload, and the belief that rest must be earned through collapse. It must include sustainability.
Rest is not the opposite of growth. Rest can make growth possible. Recovery time can protect relationships. Sensory care can reduce emotional dysregulation. Boundaries can prevent shutdown. Reduced demands can allow functioning to return. Self-validation can reduce shame and increase the likelihood that skills will be used.
Autistic burnout asks us to take capacity seriously. It asks us to stop confusing performance with wellbeing. It asks us to recognise that appearing fine is not the same as being fine.
For the autistic person, healing may involve learning to trust the body’s signals, honour sensory needs, reduce masking where possible, communicate limits, and allow rest before crisis. This is not avoidance. It is Wise Mind.
Autistic burnout can be distressing, confusing, and deeply disruptive. It can affect daily functioning, relationships, work, study, self-esteem, and emotional regulation. It is not laziness or lack of motivation. It is often a sign that the person’s capacity has been exceeded for too long.
Wise-Mind DBT Brisbane provides therapy and DBT-informed support for people experiencing autistic burnout, emotional dysregulation, sensory overwhelm, masking, shutdown, ADHD, BPD, Complex PTSD, relationship distress, and difficulties with coping or communication.
Wise-Mind Matters